Hi, everyone. Welcome to part 5 in our BLS video series, CPR for infants.
Let’s start with our initial response, which is just like in the child. What do we do first? If you witness this arrest, you saw the infant stop breathing in front of you, immediately call 9-1-1, get professional help coming, as opposed to finding the child down. Let’s say you go to check on them at naptime and you find them unresponsive and not breathing. In this case, the recommendation is you perform at least 2 minutes of CPR first, prior to calling 9-1-1. If you watched them go down, you saw the event, call 9-1-1 immediately. If you found them down, 2 minutes of CPR first, then go call 9-1-1.
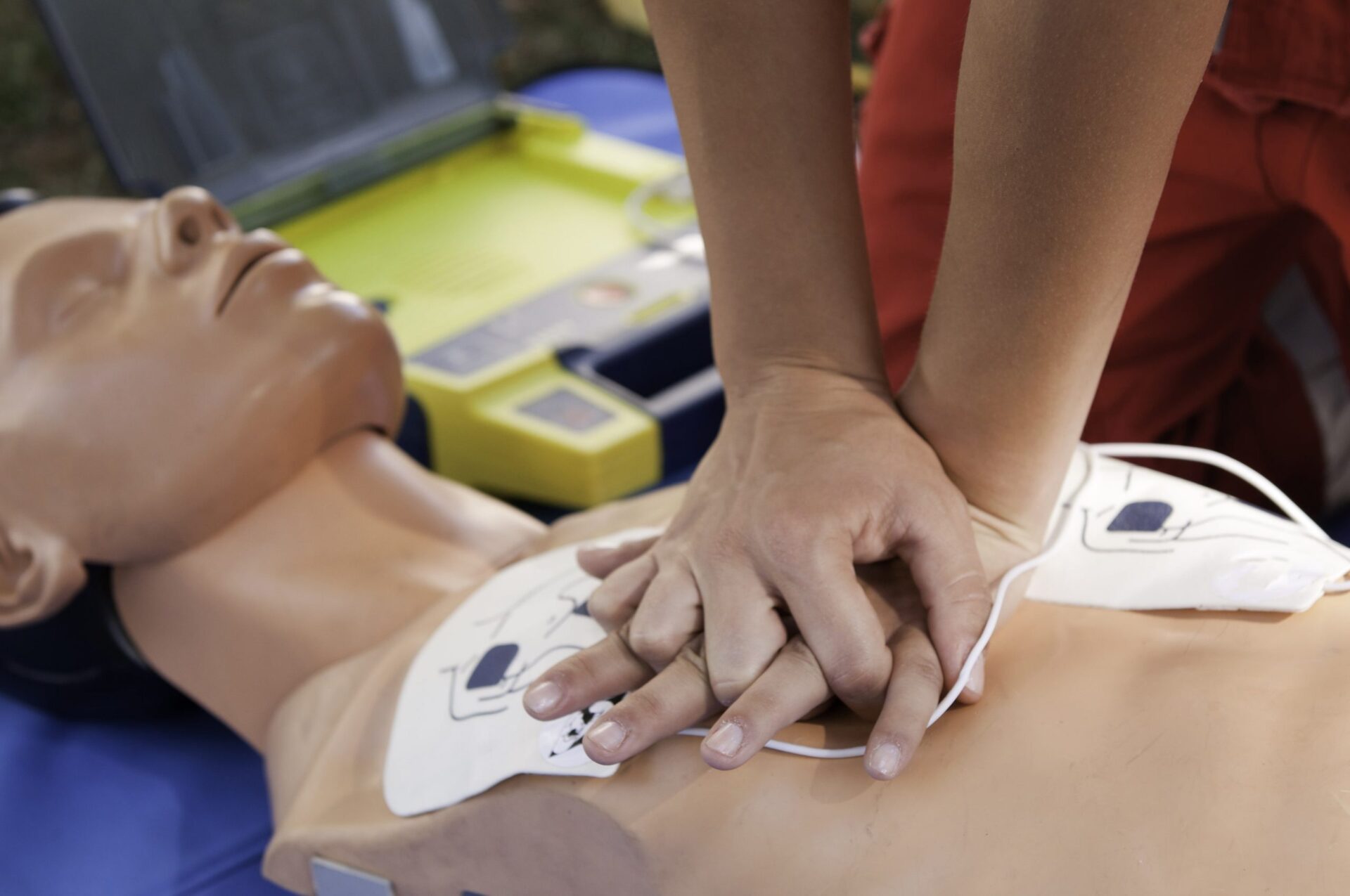
Going through the steps of our resuscitation: One, establish unresponsiveness. Poke the child. Flick the feet. You’re looking for breathing. Again, you’re either going to call 9-1-1 or you’re going to start CPR for 2 minutes, depending on whether you saw it or you found the child down. Next, check for a pulse. If you took an infant and laid them flat on their back, their arms would pop up like this, which is great because this is where you’re going to check for a pulse. In an infant, you’ll check for a brachial pulse. Slide your fingers between the two muscles in their upper arm and palpate for a pulse. You’re going to feel for at least 5 seconds but no more than 10 seconds. If there’s any question as to whether or not you feel a pulse, begin chest compressions. Next, chest compressions. If you’re alone—one rescuer—you’re going to use the two-finger technique for chest compressions. Place two fingers in the center of the chest, at the nipple line. Your compression depth is 1/3 the distance anterior to posterior. You’re going to compress about 1/3 of the distance through this kid’s chest, and you’re using the two-finger technique, which allows us to go and quickly perform our 2 ventilations and then come back and do another 30 chest compressions. Our compression-to-ventilation ratio for one rescuer is 30:2 (30 compressions, 2 breaths of air). If you have two rescuers, first, our compression-to-ventilation ratio changes. It’s going to change to 15:2 (15 compressions, 2 breaths of air). This will provide twice as many ventilations to the infant. Also, our CPR compression technique changes. Instead of using two fingers in the center of the chest, we’re going to use the two-thumbs technique. Come around the patient’s chest and put your thumbs at about the center of the chest, at the nipple line. You’re going to use your hands to compress, again, 1/3 of the distance through this infant’s chest. Compress 1/3 of the distance anterior to posterior. When performing chest compressions on an infant, it’s important that you have the infant on a flat, solid surface, especially if it’s a one-rescuer technique, so you can get adequate depth during your chest compressions. Ventilations for an infant: If it’s a two-rescuer technique and you’re using a positive pressure bag to ventilate the child, an Ambu bag, it’s important that you have a properly fitted mask. Again, the mask should cover the infant’s nose and mouth—don’t extend up into the eyes or past the chin—so you’re able to get a good seal when you provide positive pressure ventilation. Again, what are we looking for with each breath? Chest rise. You want to see that chest come up and come down with each ventilation. When performing ventilations on an infant, it is very important to properly position that infant first. In this case, you’re most definitely going to need something behind the shoulders to raise the shoulders up and get that airway in a neutral position so you can adequately perform positive pressure ventilations. Again, what are we looking for? Chest rise with each breath.
As soon as an AED arrives, attach the AED to the infant. If the machine recommends and prompts you to shock them, immediately defibrillate this infant.
This has been part 5 of our BLS video series, CPR for the infant. I’m Mark. Thanks for watching. I’ll see you in the next video.
Recommended Articles

BLS Pediatric Cardiac Arrest Algorithm – Single Rescuer
The BLS Healthcare Provider Pediatric Cardiac Arrest Algorithm – Single Rescuer shows the steps single rescuers should take in the case of an unresponsive child or infant.