Hi, everyone. Welcome to part 4 in our BLS video series, CPR for children. When we’re talking about children, the age group we’re talking about is between 1 and 8 years old. That’s the age group that defines a child.
Let’s start with our initial response because there are a couple of different recommendations. If you see the child go down, you witness this arrest, you’re at a sporting event and you watch this kid go down, the recommendation is that we call 9-1-1 immediately and we go retrieve an AED. We saw him go down, call 9-1-1, get an AED, as opposed to finding the child already down. Say you walk into a bathroom and you come across a child who’s unresponsive. In this case, the recommendation is to perform at least 2 minutes of chest compressions and ventilations prior to calling 9-1-1 and getting the AED. You see them go down, call 9-1-1 and get an AED. You find them down, 2 minutes of CPR first, then go call 9-1-1 and get an AED.
We’ve established unresponsiveness, called 9-1-1, sent someone for an AED. Next step, check a pulse and respirations, at the same time. Remember, when checking for a pulse, at least 5 seconds but no more than 10 seconds. If there’s any question as to whether or not you feel a pulse, you’re not sure, start chest compressions. Again, assess for no more than 10 seconds. Where do you check for a pulse on a kid? You can check carotid or you can check femoral. Slide your hands into the groin across from the hip bone. Slide your hands in there and try to palpate and appreciate a femoral pulse. Again, you’re not going to check for more than 10 seconds.
Next, start first with chest compressions. Our compression rate, same as an adult. You’re going to compress between 100 and 120 compressions per minute. That’s our rate of chest compressions. How far into the chest do you push? Our depth on a child, you’re going to compress 1/3 the distance anterior to posterior. You’re compressing about a third of the way through this kid’s chest. These are deep compressions. Compression-to-ventilation ratio? For one rescuer—if it’s just you—the compression-to-ventilation ratio is the same as an adult, 30:2 (30 compressions, 2 breaths of air). If there are two rescuers then the ratio changes to 15:2 (15 compressions, 2 breaths of air). The reason it is important to move to a 15:2 compression-to-ventilation ratio is because overwhelmingly the reason pediatric patients arrest in the first place is respiratory in nature. This 15:2 ratio provides twice as many ventilations.
In the adult, you’ve probably heard of hands-only CPR. The reason we can get away with that is in the adult, they probably arrested from an arrhythmia; the heart went into an arrhythmia and the adult patient collapsed. There was probably still oxygen in their bloodstream when they arrested, right? So, we can just do hands-only CPR and get away with that in the adult for a while. We can’t do that with a child because when a child arrests, it is usually respiratory in nature in the first place. By the time the kid arrests, they’re already hypoxic. They’re already depleted in oxygen, so we cannot get away with hands-only CPR on a kid. Any time you’re performing CPR on a child, compressions and ventilations.
Next, hand placement when performing chest compressions on a child. On the adult, you would have the heel of your hand on the lower portion of the sternum. If you think about it, on a small child your hand is going to take up the whole sternum, so your hand is going to go in the center of the chest. If you use one hand or two hands when performing chest compressions on a child, who cares? It doesn’t matter. You can use one hand or two hands. What is important is that we’re providing adequate depth and adequate rate when we’re providing those chest compressions. One hand, two hands—doesn’t matter. Focus on your rate and your compression depth.
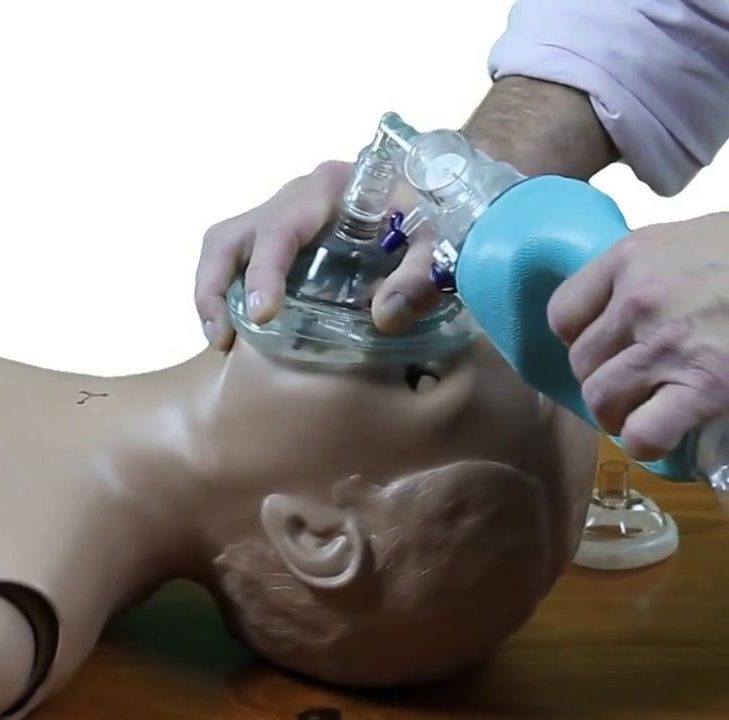
Next, a quick word about ventilating this child. If you’re using a bag valve mask, what’s important is making sure you’re using the proper size mask. The mask should fit over the nose and the mouth of the child, not extend up into the eyes or past the chin, so you’re able to get a good seal. You may need to place a towel roll underneath the child’s shoulders to raise the shoulders up and allow for that large occiput so we can get the head in a neutral position. Again, what we’re looking for is chest rise with each ventilation.
As soon as the AED arrives, attach it to the child. Assess to see if the child needs to be shocked. If they do, perform immediate defibrillation. Don’t wait. Shock that child.
This has been part 4 CPR for the child. I’m Mark. Thanks for watching. I will see you in the next video.