The common respiratory arrest definition is the cessation of breathing. Respiratory arrest is usually the endpoint of respiratory distress that leads to respiratory failure. Respiratory distress and failure have multiple causes, all of which, if left untreated, can deteriorate into respiratory arrest.
Regardless of the cause, respiratory arrest is a life-threatening situation that requires immediate management. When a patient goes into respiratory arrest, they are not getting oxygen to their vital organs and may suffer brain damage or cardiac arrest within minutes if not promptly treated.
The best treatment is knowing and understanding the signs and symptoms of respiratory distress and respiratory failure so interventions can be initiated and respiratory arrest averted altogether. Let’s take a look at the difference between respiratory distress, failure, and arrest and how to treat respiratory arrest.
Respiratory Distress
According to the American Heart Association (AHA), the following are clinical signs of respiratory distress. The patient may not experience all of them, and the level of severity will be patient dependent:
- Tachypnea
- Increased respiratory effort (nasal flaring, retractions)
- Inadequate respiratory effort (hypoventilation or bradypnea)
- Abnormal airway sounds (stridor, wheezing, grunting)
- Tachycardia
- Pale, cool skin
- Change in level of consciousness/agitation
- Use of abdominal muscles to assist in breathing
Understanding the patient is attempting to maintain adequate gas exchange while in respiratory distress in important. The inability to oxygenate and ventilate because of worsening disease or fatigue places the individual at risk for developing respiratory failure.
Respiratory Failure
Respiratory failure can result from upper or lower airway obstruction, lung tissue disease, and disordered control of breathing (AHA). The AHA stated that providers should suspect probable respiratory failure if some of the following signs are present:
- Marked tachypnea
- Bradypnea, apnea (late)
- Increased, decreased, or no respiratory effort
- Poor to absent distal air movement
- Tachycardia (early)
- Bradycardia (late)
- Cyanosis
- Stupor, coma (late)
Respiratory Arrest
Respiratory arrest is simply the absence of breathing. It can result from respiratory distress, respiratory failure, or other events including acute head injury or drowning.
Management
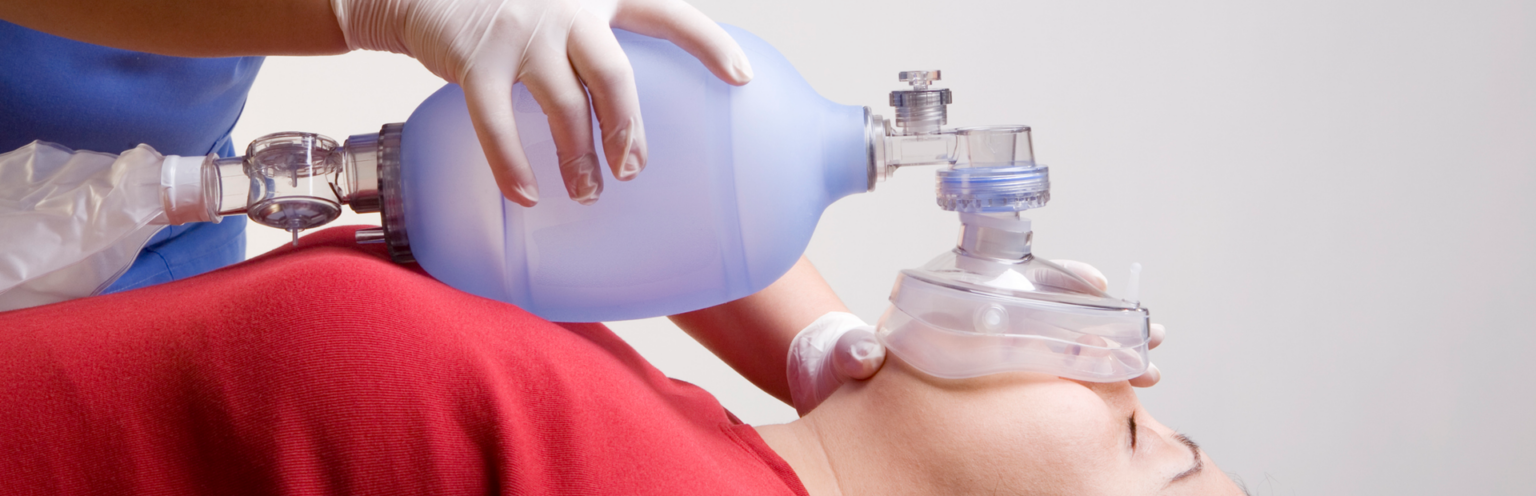
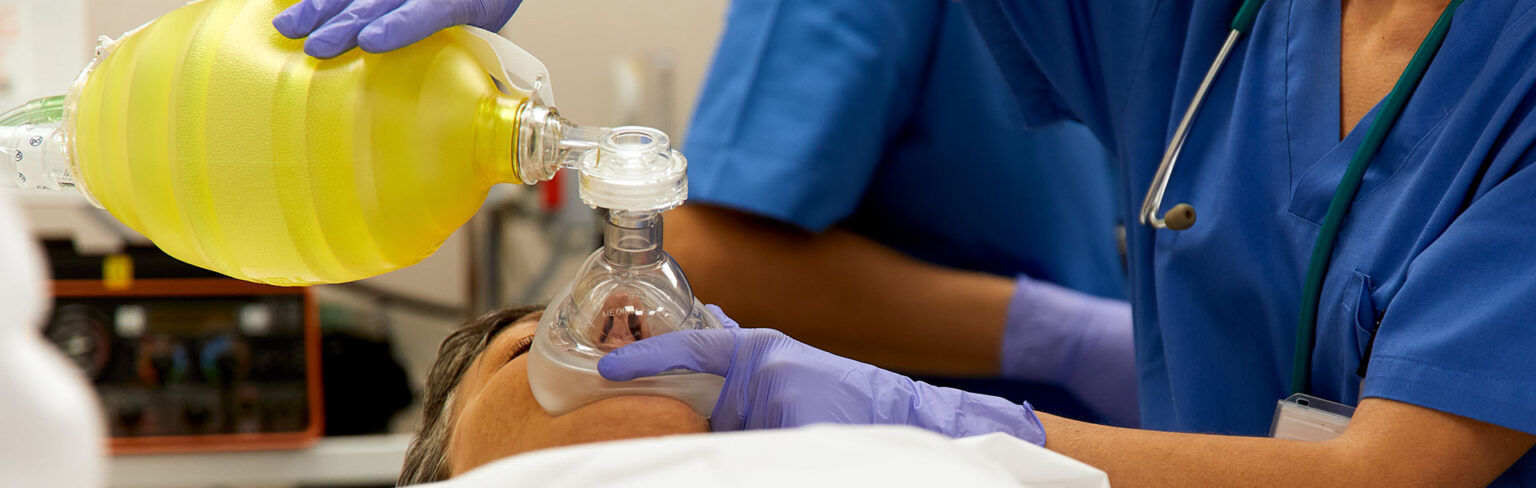
After assessing the patient and determining they are in respiratory arrest, proper respiratory arrest management requires that multiple things should happen at the same time. Help should be elicited so other interventions could be implemented, the airway should be opened, bag-mask ventilation should be applied, and preparation for an advanced airway should be begun.
Open the patient’s airway and provide positive pressure ventilation with a bag-valve-mask device. In most cases, unless the patient has a neck or spinal cord injury, you can open the airway using the head-tilt chin-lift method. If a neck or spinal cord injury is possible, the airway can be opened using a jaw thrust maneuver.
Bag-mask ventilation can be instituted with, or without, an oral or nasal pharyngeal airway. These airways help displace tissue to allow for easier ventilation and oxygenation. The use of an oral airway can be helpful in order to prevent the tongue from blocking the airway. An oral airway will cause gagging, so be sure to use one only if the patient is unconscious. In the semi-conscious patient, a nasal airway is recommended. Some patients may be very difficult to mask ventilate without an airway, and delays should be minimized when determining whether one needs to be placed.
Care should be taken to not over-ventilate the patient. According to the 2015 AHA guidelines update for CPR and ECG, for patients with a perfusing rhythm, ventilations should be delivered once every 5 to 6 seconds (AHA). Ventilating too fast or with too large a tidal volume can increase intrathoracic pressure, decrease cardiac output, decrease venous return to the heart, and cause gastric distension. Adequate ventilation can be achieved if the patient’s chest rises and falls with each manual respiration. Supplemental oxygen should be applied through the bag-valve-mask. Oxygen saturation of 94% SpO2 or higher are recommended, and if the patient is in respiratory arrest 100% SpO2 would be the ultimate goal (AHA).
If an advanced airway needs to be placed because of inadequate mask-ventilations or a deteriorating condition, there are multiple devices available. Advanced airway equipment includes the laryngeal mask airway (LMA), laryngeal tube, esophageal-tracheal tube, and the endotracheal tube (ETT) (AHA).
Prior to the patient being intubated with an ETT, you may need to suction the mouth and oropharynx in order to remove any secretions so that the vocal cords can be visualized. Confirmation that the trachea has been successfully intubated may be initially indicated by chest rise. In addition, place an end-tidal CO2 device, which will indicate the presence of carbon dioxide during exhalation. A chest x-ray can be done as soon as possible to confirm tube placement. At this point, the patient will need to be placed on a mechanical ventilator.
Determine and Treat the Underlying Cause
There are many causes of respiratory arrest. For example, drug overdoses can depress the central nervous system and lead to respiratory arrest. Certain neuromuscular diseases can cause fatigue, which eventually leads to the cessation of breathing. Airway obstruction, metabolic disorders, and strokes can also lead to respiratory arrest. Knowing the patient’s history, their chief complaint, and medications they are taking can help determine the underlying cause.
In addition, blood tests such as arterial blood gases, a complete blood count, electrolytes, and others may provide clues as to the cause of the respiratory arrest. A chest x-ray should be performed.
Resources
- American Heart Association. Advanced cardiovascular life support provider manual. Dallas, TX. 2016.
Recommended Articles
Becoming Familiar with Synchronized Cardioversion
For certain types of cardiac arrhythmias, synchronized cardioversion can be an effective treatment. Learn about synchronized cardioversion and the differences between it and defibrillation.