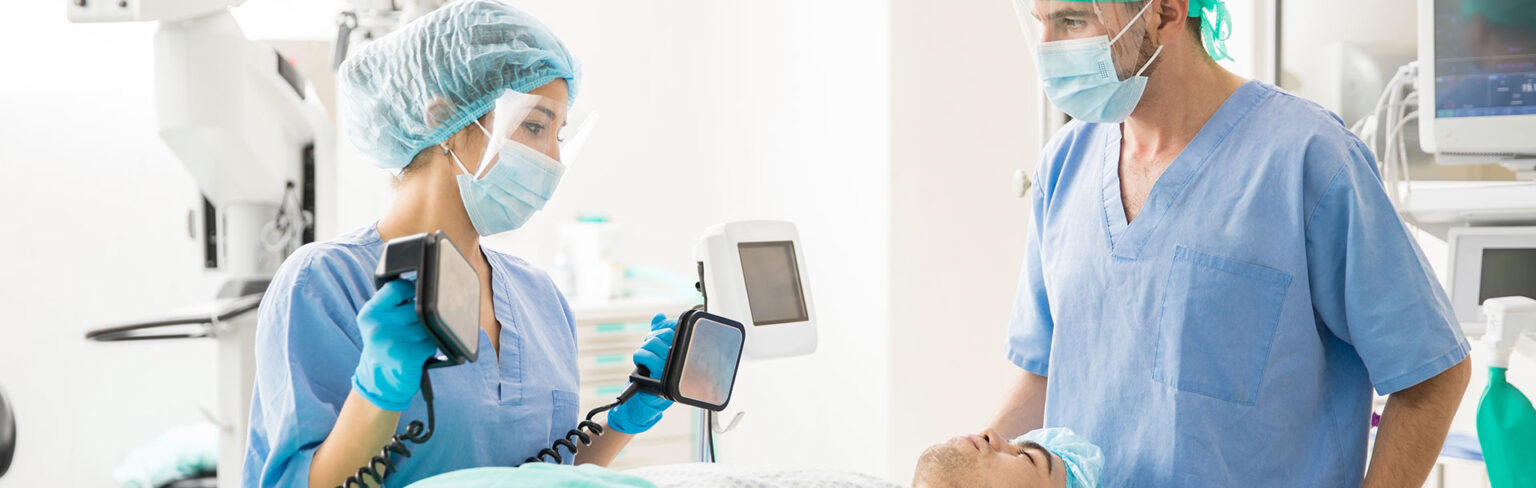
Hi. I’m Mark from ACLS Certification Institute. In today’s video presentation, we’re going to talk about end-tidal capnography—how we use it in ACLS and especially during a cardiac arrest.
What is end-tidal capnography? It’s a quantitative measurement of a patient’s exhaled CO2, which is the byproduct of cellular metabolism. I kind of think of it like the exhaust in a car. You fill the car up with gas. The motor uses the gas and then kicks out exhaust. If you get a notice from your emissions center like I just got, I’m going to take my van in and have the emissions center check my exhaust. By evaluating the exhaust, they can see if there’s a problem with the motor. This is exactly what we’re using end-tidal CO2 for in ACLS. Remember, the cells are going to use this oxygen, create the CO2, but I still have to have adequate cardiac output, a working pump, to pump that CO2 all the way back to the lungs so it can be exhaled and measured.
Usually in the field, I’m using end-tidal to tweak my ventilator. I’m using it for respiratory and pulmonary status. Remember, a normal end-tidal is between 35 and 45. I can look at those numbers and adjust my ventilator accordingly to keep them within a normal range. However, in ACLS and in a cardiac arrest, I’m using end-tidal not necessarily for the pulmonary or respiratory status but to look at the function of the pump, the function of the heart. It can also help determine the effectiveness of the chest compressions I’m doing if the heart fails.
Before we get into these numbers, let’s take a quick look at a capnography waveform and define the parts in the waveform. Remember, we’re talking about the patient’s exhaled CO2. This upward inflection we’re seeing here first is the patient exhaling. They’re blowing off CO2. The patient starts to exhale—they’re starting to blow off CO2—and we can see this waveform start to rise. Then it plateaus and levels off, and where it ends and drops is the beginning of the patient’s next inspiratory effort. Where are we actually getting this end-tidal number from? It’s the end-tidal. Remember, the one breath of air, the amount of air that a patient takes in during one breath is called the tidal volume. Whether they take the breath in or we’re giving them the breath, that’s the tidal volume, the amount of air that’s going in during one breath. Now the patient’s going to exhale all this tidal volume. We can see that they’re exhaling the tidal volume and exhaling the tidal volume. It ends and they begin to take a breath, so this is their end-tidal exhalation and that’s where we’re getting that number from. That’s the amount of exhaled CO2 during that one exhaled breath or exhaled end-tidal volume. Moving horizontally from left to right, when we’re looking at this waveform, that’s the measurement of time: how fast is the patient breathing. To demonstrate this, let’s say the patient’s respiratory rate goes from 20 to 50. You can see how the waveform has become shorter because the patient is taking less time to exhale. Again, moving from left to right horizontally, that’s the measurement of time. We’re looking at the patient’s respiratory rate and all this upward deflection is exhalation by the patient.
During a cardiac arrest, it’s our goal to achieve an end-tidal reading of at least 10 mmHg (or above 10 mmHg). If during chest compressions we notice that our end-tidal reading is at 10 or below, we need to improve the chest compressions we’re doing.
Another great benefit to continuous end-tidal monitoring during a cardiac arrest is to assess for the return of spontaneous circulation. We’re working our full arrest, we’re working our full arrest, and suddenly our end-tidal spikes to over 40. Boom, baby! We have lift off! Yep, assess the patient. We may have just had a return of spontaneous circulation. Remember, this CO2 has been building up in the body, but we’ve had poor perfusion because we’re only providing chest compressions. Suddenly the heart begins to beat on its own, it rapidly pumps all the CO2 back to the lungs, and we can read that on our end-tidal and that’s what caused the rapid increase in our end-tidal reading. If our patient has had a return of spontaneous circulation, we’re going to adjust our ventilations to achieve an end-tidal between 35 and 40; that’s our target range we’re trying to hit.
Another great benefit to continuous end-tidal monitoring during an arrest and especially in the intubated patient is breath-by-breath monitoring of that ET tube placement. If we’re bagging the patient and suddenly our end-tidal goes from 30 to zero, reassess the tube. We may have just popped out our endotracheal tube. Remember, pulse oximetry can take 30 seconds and up to 1 minute to adjust. Their saturation may still be fine, but your end-tidal waveform is going to drop right of a cliff as soon as that endotracheal tube pops out.
Quick review: Why do we like end-tidal in the full arrest?
- To assess the quality of our chest compressions
- To determine a return of spontaneous circulation in the patient
- Breath-by-breath assessment and confirmation of the placement of the endotracheal tube
Let’s take a look at how are we going to set up our in-line end-tidal capnography. Usually it’s done with an adaptor. One side’s going to fit on the endotracheal tube, just like this. The other side will fit on the Ambu bag. Then there’s an adaptor that’s going to slide onto this and go back to your monitor so it can pick up and give you your reading.
Let’s have some fun with capnography for a moment. I’ve got this hooked up to an endotracheal tube and I’m going to breathe through this tube. I’m going to create a waveform on the monitor. I want you to look at the waveform while I’m breathing through this tube. First I’m just going to breathe regular, as regular as I can, then I’m going to start breathing fast, and then I’m going to hold my breath. When I hold my breath, look at what happens to the capnography waveform but then look what happens to my pulse oximetry reading.
You don’t have quantitative end-tidal capnography? We can still use one of these guys—a colorimetric detector, which is just a fancy paper that changes color when it detects exhaled CO2. Out of the package it’s purple and when it detects CO2, it will change color to gold or yellow. Remember, gold is golden. The colorimetric detector is not 100% to verify endotracheal tube placement. It is 100% for detecting exhaled CO2. I’m working a code up on the floor, respond to a full arrest, and I intubate the patient. I place a colorimetric detector between the ET tube and the Ambu bag. It stays purple and someone says, “Hey, your tube’s not good.” Well, I know my tube was good. I saw the tube pass through the vocal cords. I had absent epigastric sounds, good bilateral chest rise, good equal lung sounds, so my ET tube placement was fine. A couple minutes into the code, while performing quality chest compressions, administering epinephrine, and running the code, suddenly it changed color, from purple to gold. What just happened? The patient had a spontaneous return of circulation. Remember, this is not 100% for ET tube placement, just for the presence of exhaled CO2.
Let’s see if we can get this to detect my exhaled CO2 and change color. We remove it from the package (don’t need that), and we can see it’s purple. I’m going to exhale through it, and we can see the paper is now changing to gold, changing to gold in color. It’s detecting the exhaled CO2 and changing color. Remember, gold is golden.
If you’re a nurse in the ER, you’re working in the ER, and you know you have a cardiac arrest coming in, get your end-tidal capnography handy and get that on the patient as soon as they hit the door.
Again, why do we use end-tidal capnography in ACLS?
- To assess the overall perfusion status of the patient
- To assess how well are we doing our chest compressions
- An ongoing breath-by-breath assessment of a confirmed advanced airway
I hope you enjoyed today’s lecture on end-tidal capnography. I’m Mark for ACLS Certification Institute. Remember to like us on Facebook and, please, become a subscriber to our YouTube channel. Thanks, and I’ll see you in the next video.
Recommended Articles